Radiologists and cardiologists at Yale School of Medicine are the first in Connecticut and among the first in the Northeast to use a new personalized cardiac test that can predict the need for cardiac catheterizations.
Patients at Yale-New Haven Hospital are the first in the region to benefit from this new technology for analyzing blood flow to the heart.
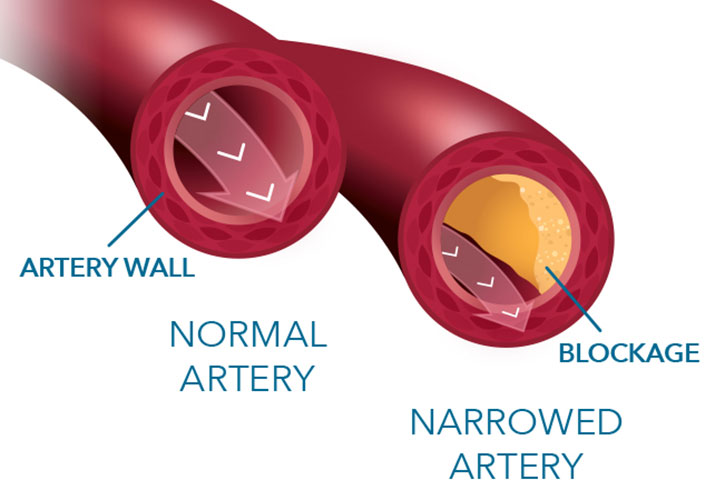
The analysis takes data from a patient’s noninvasive coronary CT angiogram -- a CT scan that looks at the heart – and creates a personalized, digital 3D model of its blood vessels. The analysis is created using powerful computer algorithms to simulate blood flow and intricately assess the impact of narrowed vessels on blood flow to the heart.
The procedure offers the potential for patients to avoid unnecessary invasive angiography (cardiac catheterization), a procedure in which a catheter is used to inject an X-ray dye directly into the heart’s blood vessels.
“The new technology already saved one of our patients from going through an unnecessary invasive procedure,” said Hamid Mojibian, MD, associate professor of Radiology and Cardiology at Yale School of Medicine.
This 73-year-old patient with chest pain also had multiple medical conditions making the cause of the pain unclear. His cardiologist had requested a coronary CT angiogram (CTA) where images from the new test clearly showed no significant arterial blockage of blood flow to the heart and excluded the pain from being cardiac in origin.
In clinical trials, this type of analysis helped identify which patients do and do not need invasive treatment.
“This new analysis is helping us develop the most appropriate treatment plan for a patient with coronary artery disease (CAD) without the need for unnecessary and stressful procedures,” said Mojibian.
Angiograms have long been the go-to diagnostic tool for CAD, the most common type of heart disease and the leading cause of death for men and women in the United States. People with CAD are at a higher risk for a heart attack and other heart conditions that can be debilitating or even fatal.
Patients with shortness of breath and chest pain often elect to undergo a coronary catheterization, But in a study reported in the New England Journal of Medicine, no coronary artery disease was found in 39.2% of patients.
“If 40% of diagnostic catheterizations in this situation are normal, we can use this new tool to make sure the right patients are getting cardiac catheterizations as quickly as possible,” Mojibian said.
This new analysis is helping us develop the most appropriate treatment plan for a patient with coronary artery disease without the need for unnecessary and stressful procedures
Hamid Mojibian, MD
“This is not for the patient with sudden crushing chest pains,” he said, “but for chest pain that lasts for a few days. These patients would usually have a noninvasive test like a stress test or coronary CTA. If the test comes back abnormal, the patient would go for catheterization.”
However, many of the tests used to determine how well a person’s heart and blood vessels are working have some false-positivity, especially in women.
“With this new test, we can reduce the number of false positives thereby avoiding unnecessary catheterizations, reducing complications, providing value and creating faster diagnosis,” Mojibian said.