He was born with the little finger," answers Jenifer, a pretty young woman with a high, bouncy ponytail, referring to her son, Matias, the wriggling baby sitting in her lap. His chubby arms and legs stick out of a onesie decorated with cars and trucks, and his big brown eyes stare, rarely blinking, at the doctors and nurses surrounding him. At six months, he's big enough to pass for 10 or 11 months.
Matias grips Jenifer’s index finger with his right hand, and she shows it to the doctors: growing alongside his thumb is a second thumb, slightly smaller than the first and moving with it.
This is the second time that Jenifer has brought Matias to Hospital Alemán Nicaragüense in Managua, the capital of Nicaragua, to inquire about removing the extra thumb. If the second thumb remains, it will not only make Matias the victim of social stigma, but it will hinder the development of his main thumb. On his first visit to the hospital, the doctors told Jenifer she must wait until he is six months old and, besides, none of the surgeons specialize in this type of surgery, especially on such tiny hands.
The hospital is a few turns up narrow cobblestone roads from the main highway in Managua. The trip on the city's packed buses cost Jenifer and Matias more than an hour; still, she made the trip once again, pinning her hopes on a rumor of a visiting group of medical professionals from the United States.
That group is Hand Help. Grant Thomson, M.D., professor of surgery (plastic) at the School of Medicine, founded the group in 2006 after seeing a need for specialized hand surgeries on other medical mission trips. Today, the group includes around 30 people: surgeons, anesthesiologists, pediatricians, occupational therapists, nurses, residents, medical students, and interpreters, over half of whom are affiliated with Yale. Once a year, the group travels to Central America to provide highly specialized hand and arm surgeries that are difficult or impossible to obtain in less-developed countries.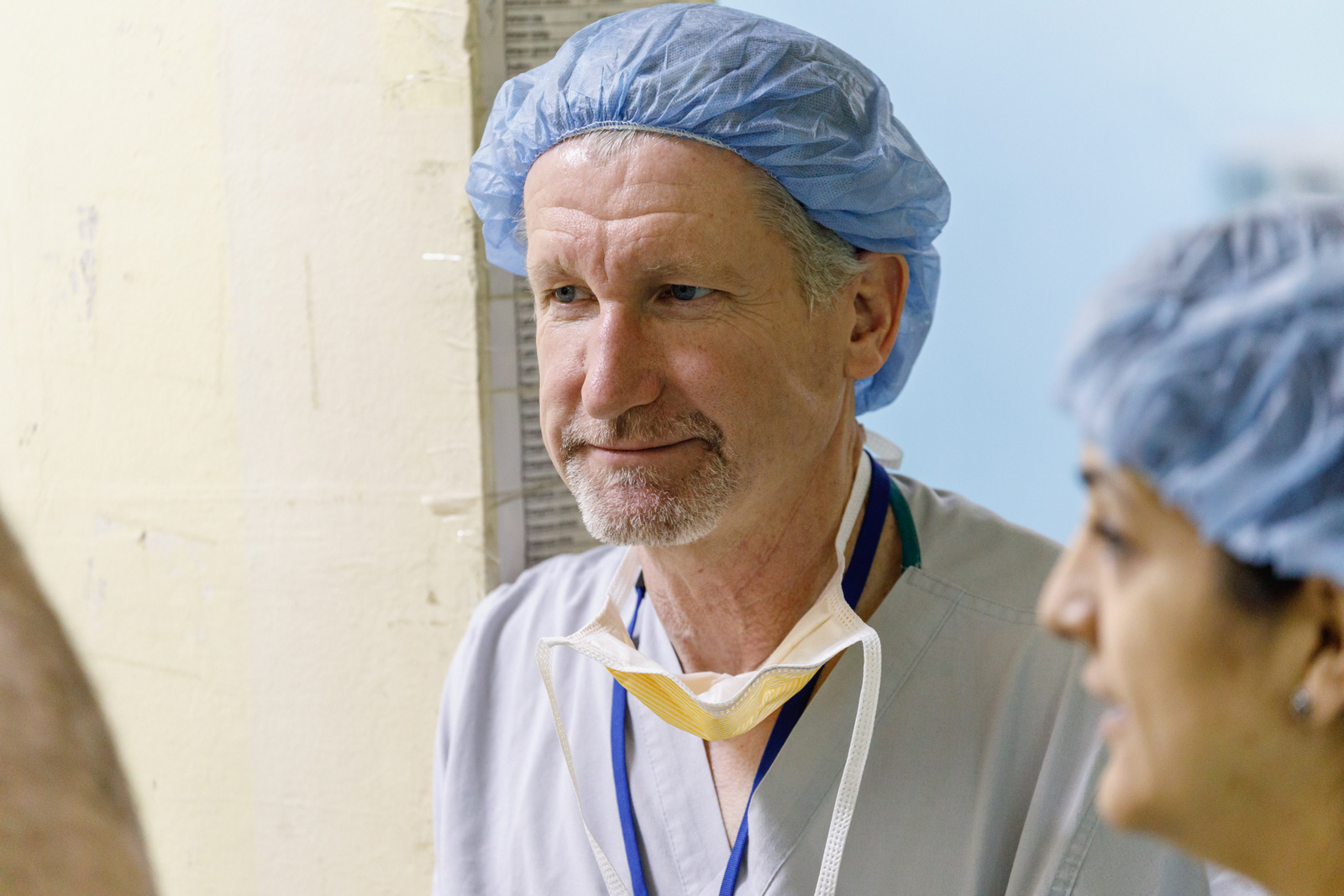
"This is medicine at its purest form,” said Kevin Tomany, M.D., an orthopaedic surgeon from Lowell General Hospital in Massachusetts, and vice president of Hand Help. “There's no preconceived notions of you receiving anything other than the benefit of healing."
Most of the surgeries are brief, allowing them to achieve those staggering numbers in such a short time. Three of the most common surgeries are removal of ganglion cysts, fluid-filled sacs typically found on wrists, which are unsightly and often painful; release of “trigger” fingers that are stuck in a bent position; and treatment of carpal tunnel syndrome, a condition in which a pinched nerve in the wrist can cause numbness and weakness. Each of these procedures typically lasts less than 30 minutes, and a Hand Help contingent can perform six or seven per day.
The overall impact on patient outcome, however, is life-changing. Nine-year-old Brigit will be able to return to school after a year away because the ganglion cysts on her wrists made holding a pencil too painful. Isabel, a 5-year-old, will be able to play and use her hands normally like other kids after the release of her two trigger fingers. Many older patients will be able to care for their children or return to work when they are relieved of the pain of carpal tunnel syndrome.
“It’s very important for the patients in Nicaragua to have access to good hand care because a lot of their livelihoods are based on their ability to use their hands,” explained Felicity Fishman, M.D., assistant professor of orthopaedics and rehabilitation at the School of Medicine. “It’s a matter of getting them back to everything they need to do to survive.”
A lesson in the art of medicine
In the United States, we don't understand that at least a fifth of the world's population doesn't have access to modern health care, that if they have a need for surgery, they can't get it.
Grant Thomson, plastic surgeon
When members of the Hand Help team board the buses that take them to the hospital each morning, most carry bottles of Fuente Pura, a local bottled water brand, stowed in their bags. Newcomers learn to save the empty bottles because, at the end of each day, a Nicaraguan nurse collects them and whisks them away to the pathology department, where they'll be used to transport samples of bodily fluids for testing. "Resources that we take for granted at home—suture, drapes, extra gloves, things like that, things at which we don't even bat an eye—we have to think twice about here," said Regina Meis, M.D., a clinical fellow in plastic surgery at Yale.Today, Nicaragua—with a per capita GDP of $5,300 that makes it the poorest country in Latin America and second-poorest in the Western hemisphere—has fewer than one physician and one hospital bed for each 1,000 people. By comparison, the United States has 2.45 physicians and 2.9 beds per 1,000 people and a per capita GDP of $54,800.
Hospital Alemán Nicaragüense, the only hospital in Managua's Xolotlán district that serves patients for free, cares for an estimated 520,000 people every year, 90 percent of whom live under the poverty line. It once received funding from the German Democratic Republic ('Alemán' means German in Spanish), which founded the hospital in 1985 as Hospital Karl Marx during the civil war that followed the Sandinista revolution against the Somoza dictatorship. At first a series of tents, the hospital slowly evolved into a sprawling compound of colorful buildings and cobblestone courtyards with East German oversight and funding. After German reunification, however, Germany backed away from funding until the Nicaraguan Ministry of Health took over entirely in 1998. Since then, the hospital has struggled with chronic equipment shortages.
“The hospital is always willing to solve, as far as we can, the population’s health problems. But because of financial matters, we don’t have the medical supplies needed,” said Fernando Aguilar, M.D., coordinator of the hospital’s orthopaedic and traumatology department. “Without the medical supplies to perform these surgeries, we can’t do anything. And that’s what happens very often in our country—we are willing to do it, we want to do it, but we lack the adequate medical resources.”
For Hand Help, this is a lesson in the art of medicine. Keeping the tight surgery schedule flowing smoothly requires the kind of adaptability that the Nicaraguan staff utilize every day. Before one surgery, for instance, the Hand Help team noticed that the arm board was significantly lower than the stretcher, meaning a patient’s arm would dangle insecurely off the bed. To solve this, a Hand Help nurse grabbed two bottles of iodine, stacked them on top of the board, and secured them in place with surgical tape.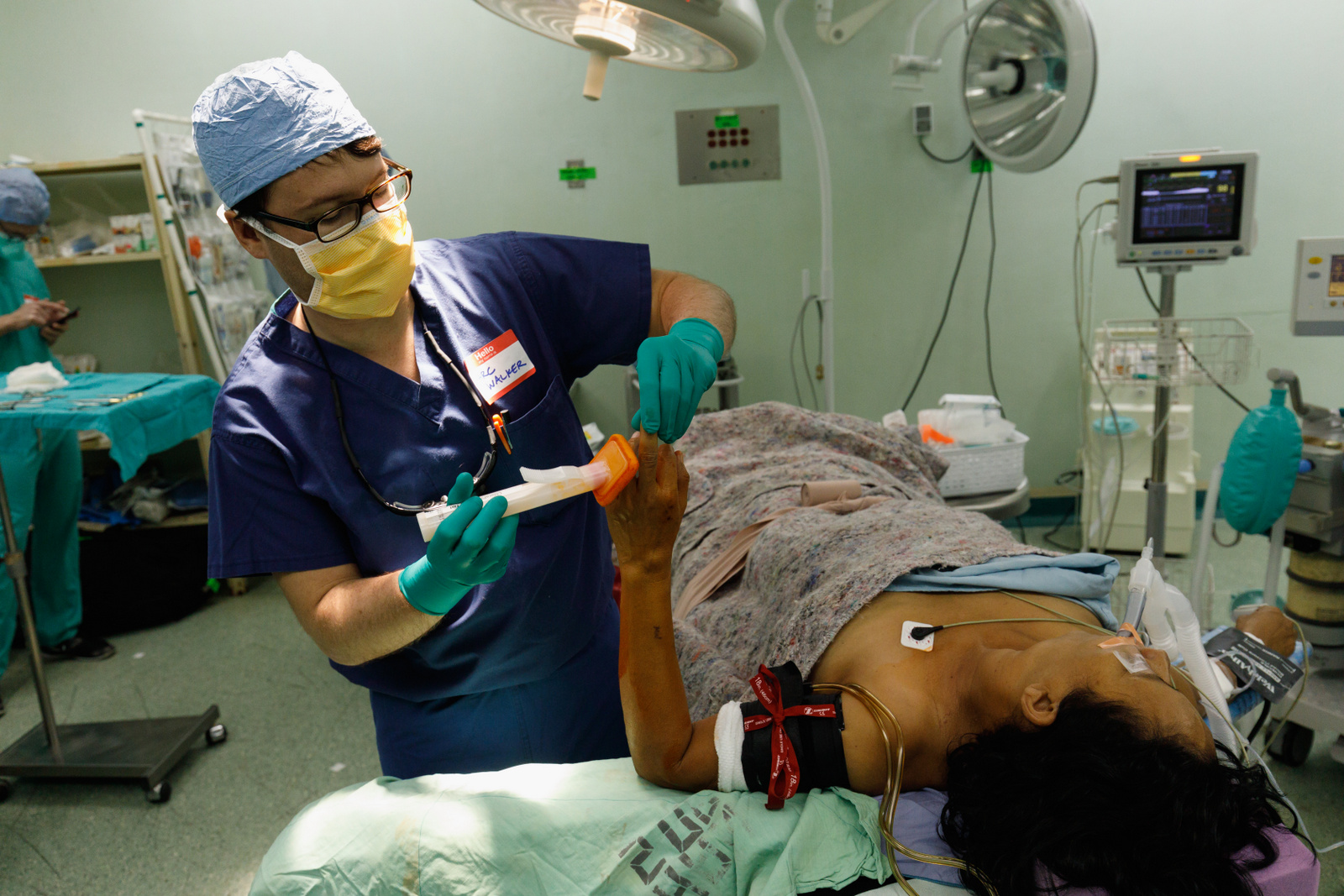
Minimizing (and maximizing) impact
To minimize their impact on the hospital’s resources, Hand Help collects donations—many from its own volunteers—to purchase all its supplies, from bandages to scissors to a machine that sterilizes equipment. Each trip costs between $25-30,000, all of which is collected without a dedicated fundraising team. For months leading up to the trip, John Tangredi, Hand Help’s secretary, painstakingly anticipates the types of surgeries Hand Help will perform and the equipment they’ll need, then packs it all into crates at a storage unit near the School of Medicine.
“We had to calculate everything we’d need from start to finish,” said Tangredi, who can list from memory the contents of each crate. “We brought 24 crates this year because we never know what they’ll have here.”
Each member of the Hand Help team checks one of the crates as part of his or her luggage. This makes for chaotic and exhausting scenes at airports—explaining endoscopic carpal tunnel surgical equipment in Spanish to skeptical customs' agents, for instance—but it’s necessary to avoid straining Hospital Alemán’s already-limited resources.
Tangredi oversees the organization and distribution of Hand Help’s equipment at the hospital from his small room in the middle of the operating suite, which he nicknamed “the kitchen.” Nurses stop by to collect tools from the bags of equipment that line the walls, Tangredi teaches fellow volunteers how to use the sterilizing machine, surgeons examine X-rays, and medical students review mnemonic devices to remember all the bones in the hand. Amid the hubbub, Tangredi wraps equipment into packages specific to each of the day’s surgeries, much as he used to do before he retired from his job as head nurse at the Smilow Cancer center and Yale New Haven hospital.
All this effort, Thomson said, helps reassure the local staff of Hand Help’s high standards. When the group first came to Nicaragua four years ago, the staff were hesitant—would the group operate the way they do in the United States, or would they merely use Nicaraguan patients to teach their medical students and residents?
“It took them a few days to realize that we were doing it the exact same way we do it in the United States, and I think that built a trust with them,” Thomson explained. Each of the four operating rooms is led by a fully-qualified surgeon and anesthesiologist, with a team of fellows, residents, nurses, and medical students assisting or watching. They are supported by the tireless efforts of Tangredi and Co. in the kitchen and the Nicaraguan staff, and they almost exclusively use the equipment they brought from the United States.
“Our mission is to recreate a surgical environment like we have in the U.S.,” explained Marc Walker, M.D., a fifth-year plastic surgery resident and organizer for Hand Help. “I think that’s unique in that, while it’d be easy to cut corners, we find that we don’t have to … and we pride ourselves on that.”
Cross-cultural efficacy and efficiency
It's March 17, the last day of surgeries. Nicaraguan and U.S. staff alike zip around the halls, exchanging equipment and the occasional bilingual joke. They've fallen into a rhythm over the previous four days, but today is St. Patrick's Day, so everyone is sporting a green bowler hat or a plastic four-leaf clover necklace, or stick-on mustaches in the color of the Irish flag. This spirited frivolity is thanks to Tangredi, Hand Help’s official secretary and unofficial establisher of cross-cultural bonding.
“It breaks the ice and opens up avenues of ‘Hey, this person is friendly; we know who to contact when we need something,’” Tangredi said of his antics, which, along with holiday decorations, include energetic hand gestures, laughter at flubbed Spanish, and plenty of candy and bubbles to curry favor with Hand Help’s youngest patients.
For those times when more formal communication is needed, however, a team of interpreters and the few members of the Hand Help team who are fluent in Spanish step in.
“It’s nice to be able to interact with the patients—to make jokes in their language so they feel more empathy and more comfortable in that environment,” said Jack Kanouzi, M.D., a postdoctoral fellow from Spain. Kanouzi and a few other Hand Help members worked double-duty as medical professionals and interpreters, from initial patient intake to the operating room. “We really want them to feel comfortable and happy, and I think knowing their language is really important for overcoming sociocultural barriers.”
More important still is accurate communication of medical procedures and outcome expectations to patients, especially because Nicaraguan patients, according to Meis, tend to be more deferential to the doctors and ask fewer questions than a typical patient in the United States. This became clear on the first day, when hundreds of potential patients came to the hospital’s clinic to be evaluated. “This woman had a small deformity on her finger that was painful, and even though someone had gone through the explanation of what we were going to do, it somehow got lost in translation and she thought we were going to amputate her finger,” Meis recalled. “Because I speak Spanish, I was able to understand the reason for her anxiety … I said ‘no, no amputation!’ and she looked so relieved. She started crying and threw her arms around me. We were able to really help her—she got to keep her finger and we took away the pain she was having.”
The rest of the Hand Help volunteers pick up a little Spanish. But it’s the long hours in the operating room, the particulars of which are familiar to both staffs regardless of language, that really help the combined teams to fall into a rhythm—respectful silence when the anesthesiologists intubate a patient, for instance, or spontaneous dance breaks between surgeries to whatever pop music plays over a nearby Bluetooth speaker. Shakira, requested by 9-year old Brigit for her pre-surgery tunes, was a particularly popular choice.
“It’s true that we speak different languages, but we can identify with each other anyway,” said Marta Hernández Ortega, a specialist nurse and chief of the local surgical technicians. “Although they can’t understand me, we’ve gotten along, we’ve worked together, and we’ve done things the best we could to help my country.”
This teamwork is crucial both during Hand Help’s hectic surgery schedule and after the team leaves, when patients need follow-up and postoperative care. In choosing a site, Thomson looks for teams of doctors and nurses who commit to both of these phases. "It's not just a matter of doing our surgery, then taking off," Thomson said. "Patients need follow-up. That's one of the most important factors—having a host that can provide support services while we're here, and also after we leave."
For its first trip in 2006, Hand Help traveled to Honduras because of its medical need and proximity. While a need for Hand Help’s skills exists around the world, the group tries to maximize the efficacy of their budget and time—a relatively cheap three-hour plane flight from Miami to Honduras means more money to bring vital equipment than if the group went elsewhere. After the continuing fallout of the 2009 Honduran constitutional crisis and military coup made working at their usual site too risky, however, Hand Help forged a new partnership with Hospital Alemán Nicaragüense in 2013. It had the trappings of medical mission success: it’s close to the continental United States and has a reputation for providing high-quality care to Nicaragua’s poorest citizens free of charge. Most importantly, its staff were eager to provide the necessary accommodations for Hand Help’s success—preparing operating suites, submitting government paperwork, contacting potential patients, and more.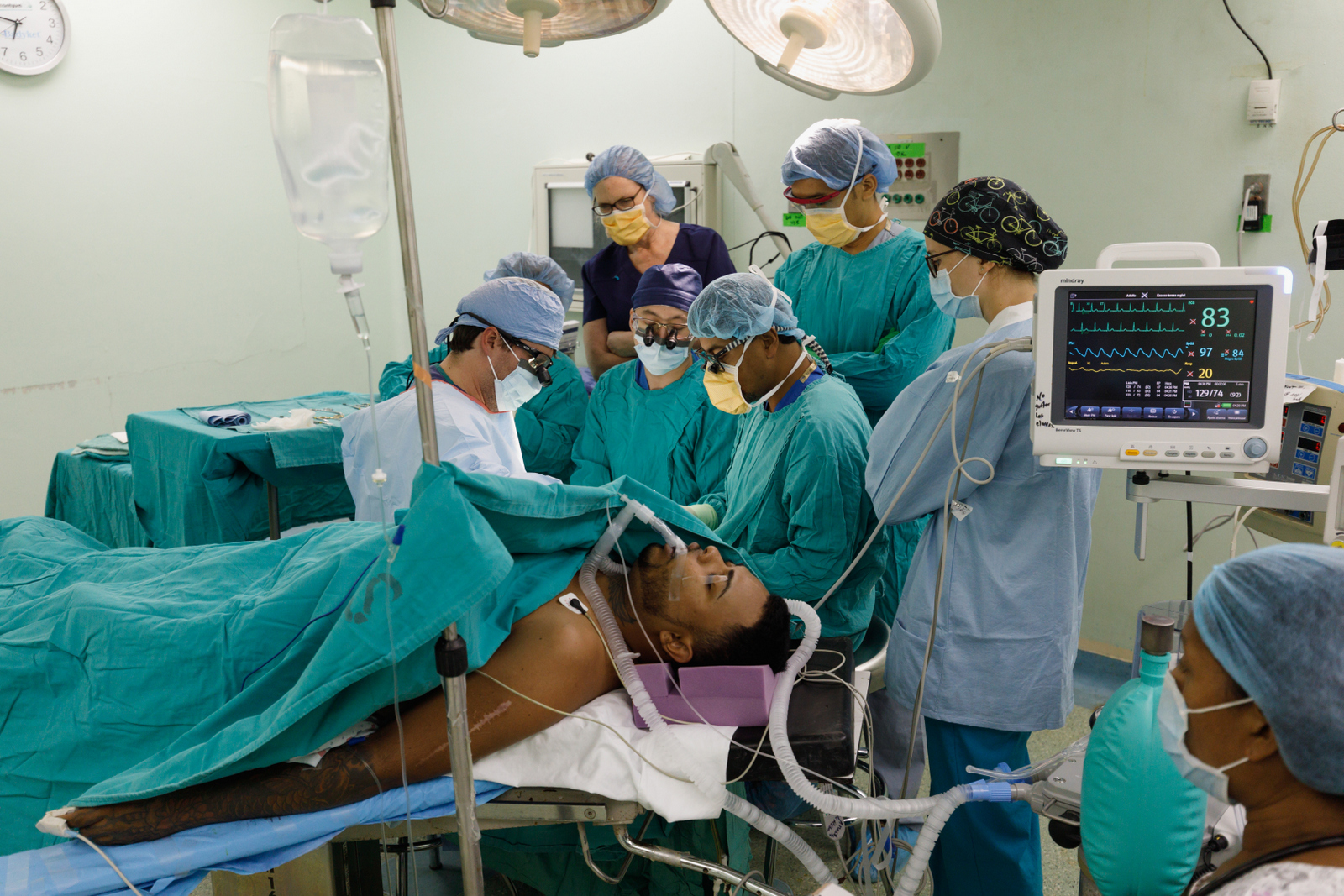
“There’s a whole team of people here who work tremendously to provide this site for us to work,” Thomson said. “They spend a lot of time working on it, which they don’t have to do, but they feel a sense of obligation to the patients.”
This obligation continues after Hand Help leaves, as post-operative care is critical for successful patient recovery—“the most important part,” as several Hand Help doctors emphasized in interviews.
“When the brigade [the hospital staff’s nickname for the U.S. contingent] comes, we perform surgeries, but then there’s the rehab processes. And in these, we see the joy that comes from those who have had surgeries,” explained Héctor Hernández, M.D., chief of Hospital Alemán’s physiotherapy department. “They recover their spirits and their lives have changed. It’s wonderful.”
Hernández and his team work with Virginia Ells, Hand Help’s occupational therapist, to curate therapy specific to each patient. In a teal building around the corner from the operating suite, Ells works long days with one of the hospital’s physiotherapists, Nubia Mayorga. They frequently lack the help of an interpreter, all of whom are busy in the operating rooms, but they deliver care anyway, making splints and teaching patients exercises with hand gestures and a lighthearted willingness to persevere.
“It’s true I can’t speak English, but I can communicate,” Mayorga said. She’s more than a foot shorter than Ells, and her bald head is covered with a pink knitted cap that she made herself. Mayorga was diagnosed with breast cancer in October and she is currently receiving chemotherapy treatment, but she came back to work with Ells and the Hand Help team.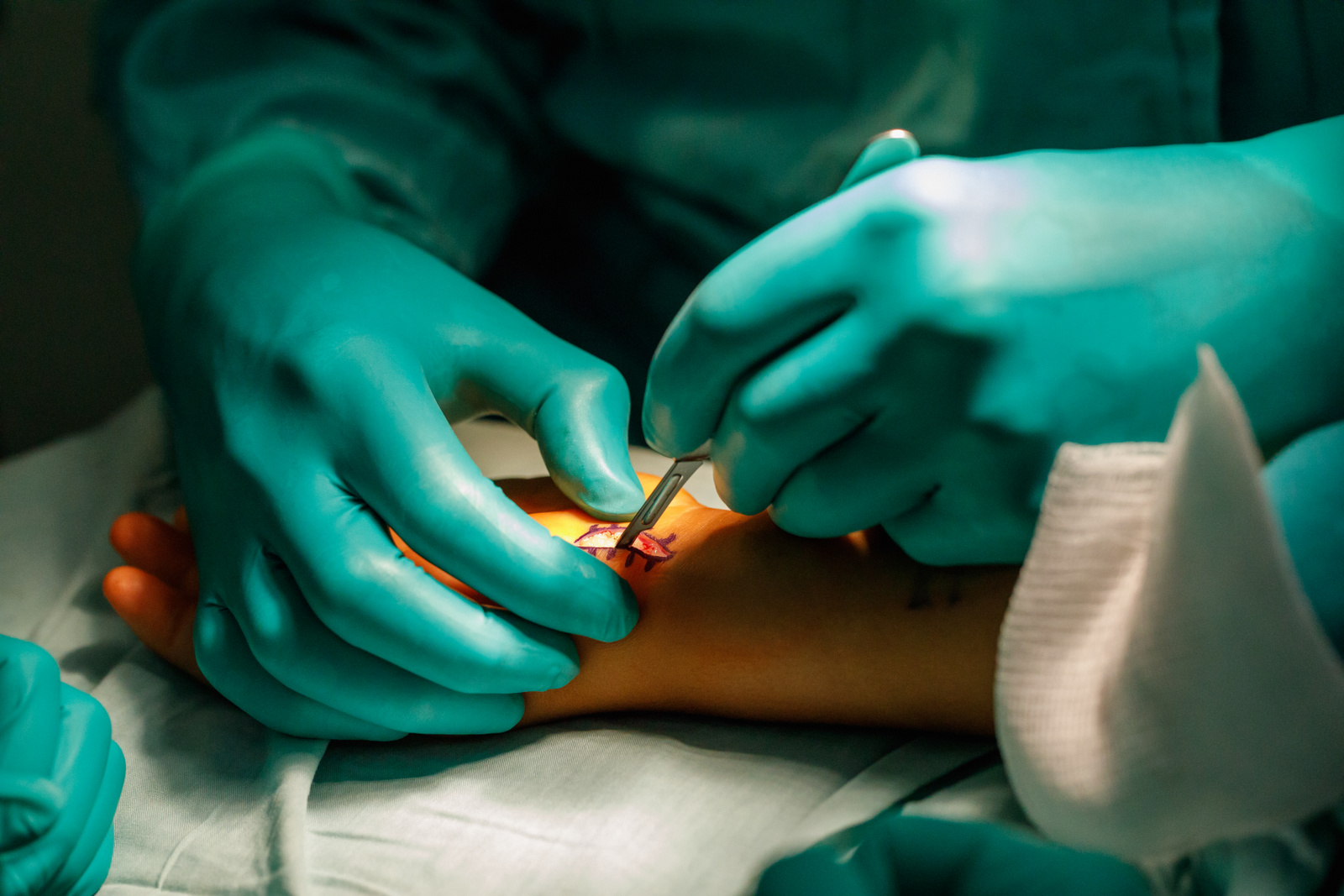
“I’ve been working with the brigade for three years,” Mayorga said cheerfully, putting her arm around Ells. “When the brigade is here, I’m here.”
Making missions “last forever”
“In the late 1990s and early 2000s, there was controversy about whether people should be doing these missions at all. There were questions of outcomes and concerns of being paternalistic,” Thomson said. “I realized Hand Help had to be different.”
Thomson uses a dual approach to avoid these pitfalls: educating local hospital staff on new procedures and studying the long-term results of Hand Help’s surgeries.
On Friday, the last full day of Hand Help’s mission, Thomson gave a lecture on endoscopic carpal tunnel release (ECTR) to a crowded auditorium of doctors, students, and residents. In this surgery, doctors insert a tiny camera attached to a thin tube into a small incision in the wrist and locate and cut the transverse carpal ligament, thereby relieving pressure on the median nerve. This method is growing in popularity due to its minimal invasion and faster recovery times as compared to earlier methods.
The Hand Help team had brought an ECTR machine, so a few staff members had seen the surgery throughout the week: Thomson looking at the video screen to navigate his tools through the small incision, chatting with the still-conscious patient, and sewing the incision closed, all in under 30 minutes. At the lecture, he explained the technique to the rest of the hospital community through an interpreter, with only one failed translation (a pun, the caption of a cartoon of two anthropomorphized mountains with roads tunneled through them: “I have carpool tunnel syndrome” laments one mountain to the other. Only the U.S. staff laughed).
Thomson guessed that this was the first time endoscopic carpal tunnel surgery had been done at Hospital Alemán, and perhaps in all of Nicaragua. Because of a shortage of trained medical professionals, most doctors gravitate towards more general specialties, leaving too few people to cover such specialties as hand surgery.
“It’s not like medicine here is different. They’re practicing advanced medicine, but the things that we bring augment that,” explained Walker, who, after completing a surgery, often chats with Hospital Alemán’s residents about the particulars of the surgery. “That knowledge-sharing component is how we can make the mission last forever.”
Additionally, in Hand Help’s early years, Thomson took pains to assess the efficacy of Hand Help’s trips. He recruited medical students from the United States to return and examine patients four and six months after surgery for two consecutive years, an uncommon practice in the medical mission world. In addition to finding a few ways to improve outcomes, the volunteers ultimately discovered that, in the long term, Hand Help’s missions improve both hand function and overall quality of life for the patients.
“It does turn out that the way we do things is helping people,” Thomson said. He is currently publishing his research, which is the first of its kind.
Sohel Islam, M.D., a plastic and surgeon, and one of Thomson’s previous Yale Hand Fellows, from Danbury, Conn., and Robert Golenbock, M.D., a pediatrician at Danbury Hospital, enter the room where Jenifer and Matias wait, accompanied by a doctor and nurse from the hospital. Islam and Golenbock greet Jenifer in halting Spanish and coo over Matias as they inspect his thumbs. In English, they discuss when to squeeze him into the surgery schedule—tomorrow morning, in Islam’s operating room. Golenbock blows a raspberry at Matias, who promptly slaps the doctor's face—his tiny, smooth hand with its little finger momentarily contrasted against the five-o-clock shadow on Golenbock's cheek.
“Are you happy?” one of the nurses asks Jenifer the following afternoon. She’s cradling Matias closely to comfort him—he’s cranky, having just woken up after his hour-long surgery to discover a heavy cast covering his right arm from his fingertips to his elbow. It will come off in one month, after which Matias will look and develop like any normal baby.
“Yes, I’m happy,” she responds, smiling.