When Frank Minja, MD, traveled to his native country of Tanzania, East Africa in 2014 to help improve radiology services at the Muhimbili National Hospital campus in Dar es Salaam, he knew the task would be complex and demanding. Minja, an assistant professor of neuroradiology in the Department of Radiology & Biomedical Imaging at Yale School of Medicine (YSM), established the Yale Radiology Global Outreach Program that year to help address the shortage of well-trained diagnostic and interventional radiologists around the world.
In a country with limited resources such as Tanzania, patients have little or no access to the benefits of interventional radiology (IR) because not a single radiologist in Tanzania had been formally trained to use it, said Minja. IR is a minimally invasive procedure that allows doctors to treat complex medical conditions and diseases through tiny holes in the skin. It is especially useful for treating patients with end-stage cancer when surgery is no longer an option.
“We organized a very successful fundraising campaign which allowed Dr. Minja and his team to achieve many positive results in a very short time. I believe our Global Outreach Program truly reflects the ideals and aspirations of the department,” said Rob Goodman, MD, chair of the Department of Radiology & Biomedical Imaging at YSM.
Minja has returned to Tanzania at least twice a year to help train radiology residents at the Muhimbili University of Health and Allied Sciences (MUHAS). In 2017, he traveled with Fabian M. Laage-Gaupp, MD, a third-year radiology resident at YSM to perform an IR readiness assessment as part of the Global Outreach Program.
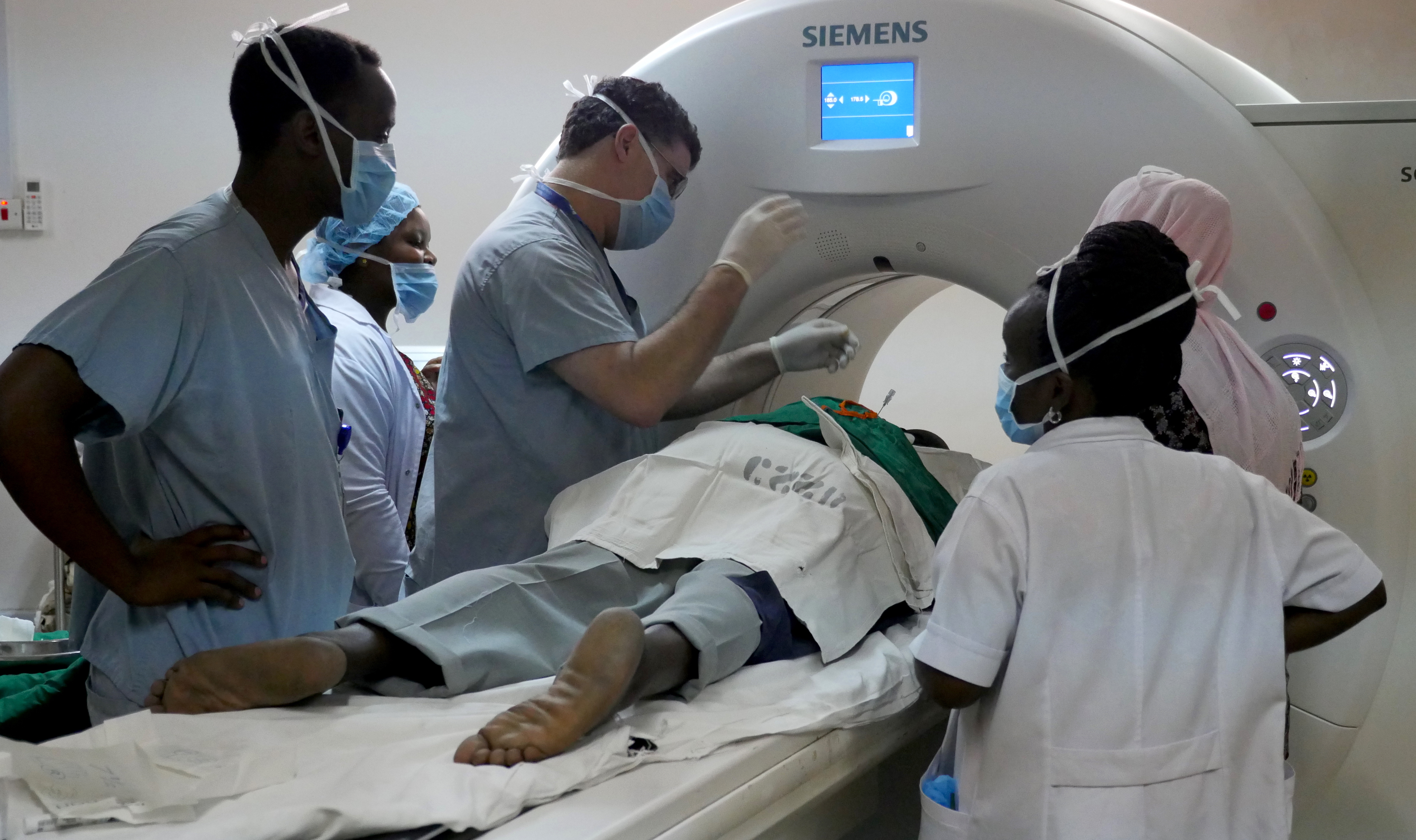
The assessment found that most of the imaging equipment needed for IR was already available at Muhimbili National Hospital (MNH), such as ultrasound, X-ray fluoroscopy, and CT scanners. The critical missing component was the lack of IR training opportunities. The Tanzania Interventional Radiology Initiative was formed to address this need and to provide within-country training for the first generation of interventional radiologists in Tanzania, graduating the first class by 2021.
“If we are able to do that, we will produce locally trained IR physicians who understand the necessary workarounds in a resource-limited setting, as opposed to training them at Yale or elsewhere abroad where more resources are readily available,” Minja said.
Assembling the First Teams
After performing the IR readiness assessment, and developing a plan with Minja, Laage-Gaupp began recruiting volunteer team members from across the United States. He recruited volunteers through presentations to the YSM Department of Radiology & Biomedical Imaging, the Global Outreach Program’s website, and RAD-AID International, as well as on Twitter, Facebook and Instagram.
Laage-Gaupp also presented results of the IR readiness assessment, and the overall IR plan, at the Society of Interventional Radiology’s 2018 annual meeting in Los Angeles. Pre-trip planning took place mainly on the WhatsApp messaging platform, through email, and conference calls.
After a year of planning, Minja and Laage-Gaupp were ready to inaugurate the Tanzania Interventional Radiology program. Together with a team of 17 doctors, nurses and technologists from YSM and other institutions they traveled to Tanzania again this past October.
“While the Tanzania Interventional Radiology Initiative had been detailed and expanded in our minds extensively over the course of a year, it remained purely theoretical until we arrived in Tanzania this past October,” Laage-Gaupp said. “To our knowledge, nobody has attempted to start an IR training program from scratch in a resource-limited setting such as Tanzania. This meant that we had no precedent to rely upon and no experts to consult.”
Yale’s IR team made good progress during its first few days in Tanzania. “Every day went a little smoother, the team grew stronger, and everyone learned from each other at an astonishing pace,” Laage-Gaupp said.
Transfer of Knowledge
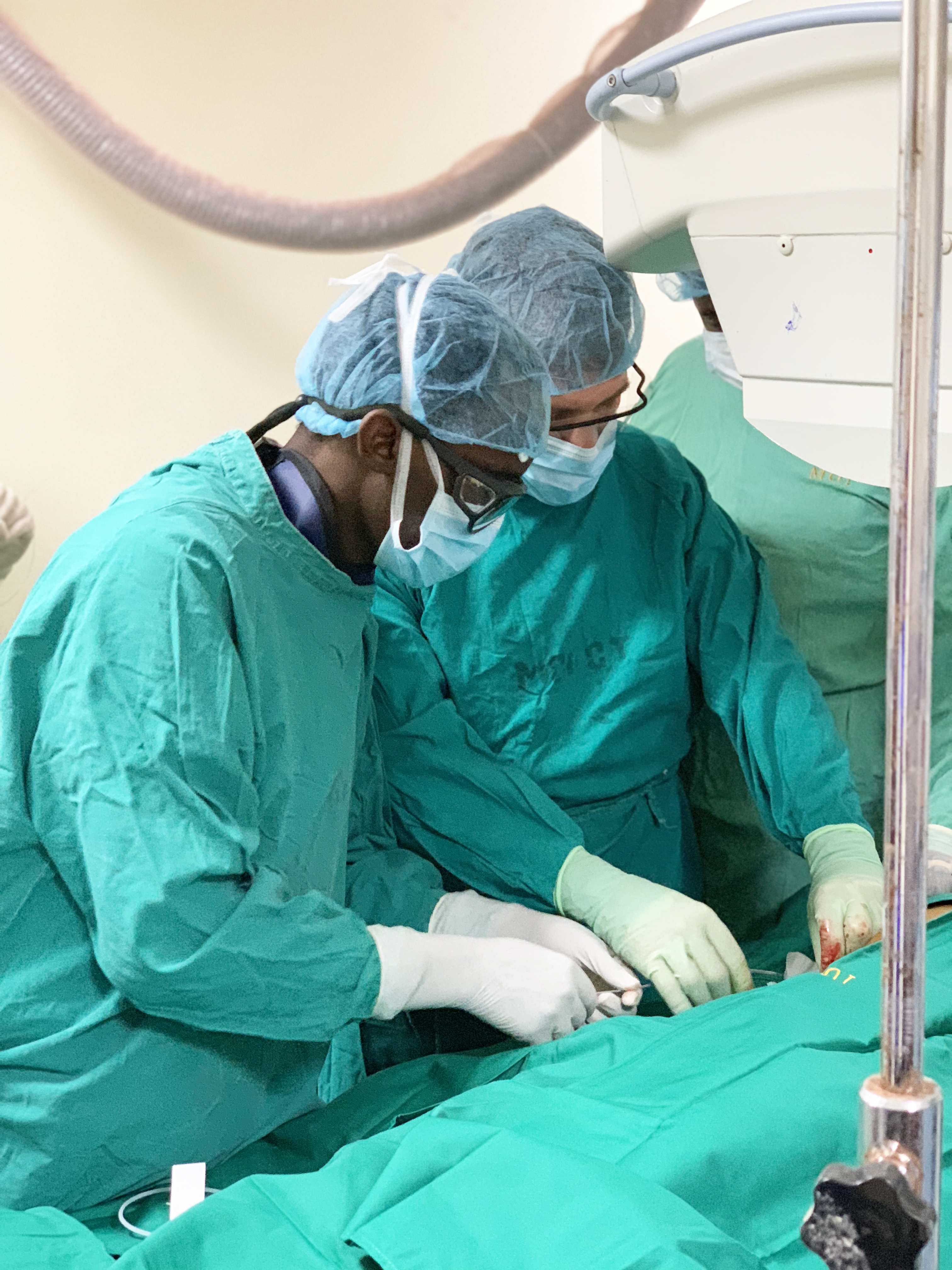
Douglas Silin, MD, assistant professor of radiology and biomedical imaging at YSM, led the first IR team at MNH. Silin’s goal was to teach the Tanzanian residents how to first do basic IR procedures “so they could do them autonomously and build their skills.” However, when he arrived at MNH, he realized that the Tanzanian team had preselected some complex cases on which to train.
“When you are developing a practice, you want to prioritize cases that have good, positive outcomes,” said Silin. “Down the road you can tackle more complicated cases.” After a couple of days, the teams were able to prioritize which cases to focus on. “They came to an understanding of this quickly,” Silin said.
David Prologo, MD, associate professor of radiology at Emory, led the second IR team at MNH. Prologo said the ability to build lasting relationships is what drew him to volunteer with the team. “What Frank and Fabian are doing is building a program that will go on for years,” Prologo said.
The Tanzanian residents quickly learned the IR techniques that he and Silin taught, which gave Prologo time to review with them processes for pre- and post-procedure patient care. Prologo plans to return to Tanzania in the fall of 2019. “I’m excited to see the progress they will make in the nine months while I’m away,” he said. In the meantime, he plans to work on a process for supplying MNH with IR disposable equipment, such as needles and catheters.
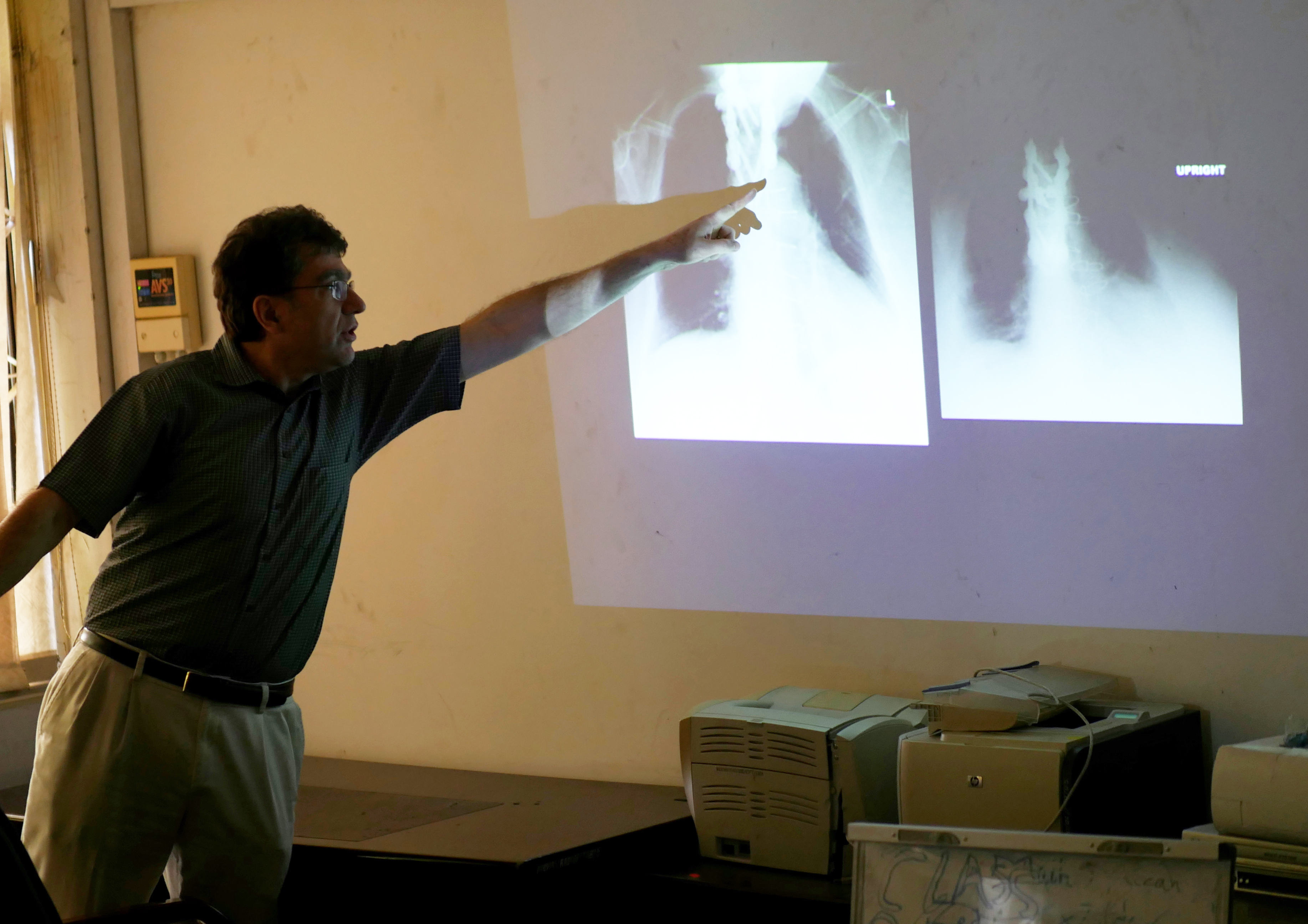
In addition to the Tanzania Interventional Radiology Initiative, the team continued to support radiology resident training at MUHAS. Timothy Rooney, MD, assistant professor of radiology at Dartmouth, was instrumental in co-leading the diagnostic radiology teaching sessions while the rest of the team was busy in IR.
“As a breast imager, I was able to share my knowledge and experience with MUHAS radiology residents who are so motivated to improve outcomes for women suffering from breast cancer,” Rooney said. “While they lack access to the technology we take for granted in the U.S., they are talented and passionate about breast cancer diagnosis and treatment. I can see that this group of residents will be instrumental in improving breast cancer outcomes in Tanzania.” Rooney plans to return to Tanzania with Dartmouth residents in the winter of 2019.
“Our faculty and residents often expressed how exciting and demanding it was to teach radiology in a different environment where many U.S.-centric assumptions about trainees and local disease patterns were constantly challenged,” Minja said. “Many of us come to Tanzania as teachers, and leave as renewed learners.”
Early Success in Numbers
The IR team’s most memorable patient was jaundiced and suffering from severe itching from accumulated bile due to the blockage of natural drainage by a surgically inoperable tumor, Minja said. “The next morning, following successful biliary drainage (a first in the country!), our patient remarked gratefully that this was the first time she had been able to sleep in weeks without itching,” Minja said.
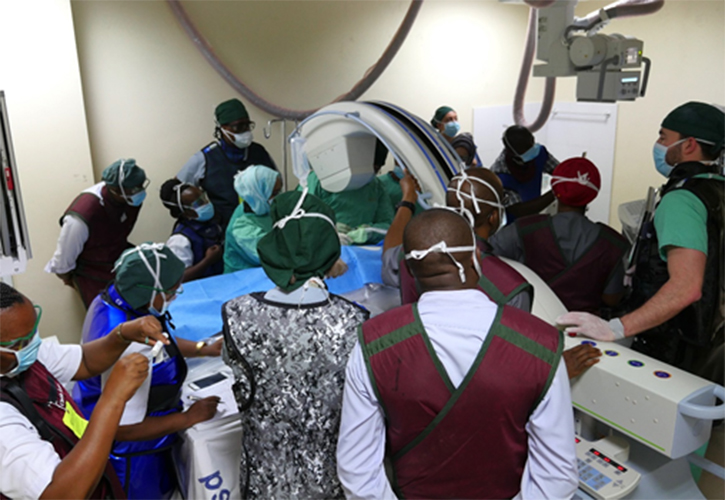
“We had a very successful launch of the Tanzania Interventional Radiology Initiative, which seeks to both train IR specialists and provide IR services within Tanzania for the very first time,” Minja said. “Over three weeks, from Oct. 21 to Nov. 9, we rotated two full IR teams at MNH. We successfully performed 37 IR procedures on 31 patients without any major complications. These procedures included biliary drainage, nephrostomy for urinary obstruction, abscess drainage, and core-needle biopsies.”
“We also started the formal training of seven MUHAS radiology residents, three senior and four junior residents, who are slowly being transformed into IR fellows,” Minja added. “We also had several visiting radiologists from other hospitals in Tanzania who were keen to observe and learn IR procedures.” Those hospitals included Muhimbili Orthopaedic Institute and Comprehensive Community Based Rehabilitation in Tanzania (CCBRT) in Dar es Salaam, and Benjamin Mkapa Hospital in Dodoma.
IR Teamwork
During his outreach trips, Minja had heard about the urgent need for IR services from Lawrence Museru, MD, executive director of MNH, Praxeda Ogweyo, MD, director of clinical support services at MNH, and Flora Lwakatare, MD, head of the radiology department at MNH. Now, with their full support, the Tanzania Interventional Radiology Initiative was able to collaborate with many departments at MNH.
“IR naturally requires a multi-disciplinary team to deliver the most effective patient care,” Minja said.
Surgeons welcomed the IR collaboration as a means for providing care to their patients. The anesthesiologists provided moderate sedation, while the emergency department helped to assess a patient who returned to the hospital with pain following a biopsy. That patient was able to return home the same night with extra pain medication.
IR also helped to provide core-needle biopsy samples to the pathology department, which are preferred to fine needle aspiration samples because of their higher diagnostic value, Minja said.
“What we didn’t realize until now is that MNH has a vision to establish liver transplantation services at the hospital by the year 2022, and robust IR services would be necessary to care for these very complicated cases,” he added.
Next Steps
A total of 10 IR teams are signed-up for 2019, with the next teams scheduled to leave for Tanzania in February. The Tanzania Interventional Radiology Initiative aims to support the cost of airfare and housing for each volunteer IR physician, nurse and technologist. Volunteers, however, are expected to pay for their visas, vaccinations, and food, Minja said.
“We have been very fortunate so far to have received many generous individual donations and two physician travel grants from the Doximity Foundation. These donations have allowed us to cover airfare costs for our two IR nurses and IR technologist. Muhimbili National Hospital also generously provided housing for eight of our 17 volunteers,” Minja said.
“There are two things we can always use more of to support our initiatives, more goodwill and more funding,” Minja said.
“Both are essential to recruit and support the best teams for the Tanzania Interventional Radiology Initiative. Many countries around the globe face an acute shortage of diagnostic and interventional radiologists, especially in Africa, and could benefit from efforts similar to the Yale Radiology Global Outreach Program,” he said.
“The problem is not very complex, but the scale and urgency of the need is quite enormous,” Minja said. “That is also the opportunity.”
We had a very successful launch of the Tanzania Interventional Radiology Initiative, which seeks to both train interventional radiology (IR) specialists and provide IR services within Tanzania for the very first time.
Frank Minja, MD, Department of Radiology & Biomedical Imaging at YSM